Abstract
Background: The COVID–19 pandemic is dominated by variant viruses; the resulting impact on disease severity remains unclear. Using a retrospective cohort study, we assessed the hospitalization risk following infection with seven SARS-CoV-2 variants.
Methods: Our study includes individuals with positive SARS–CoV–2 RT–PCR in the Washington Disease Reporting System with available viral genome data, from December 1, 2020 to January 14, 2022. The analysis was restricted to cases with specimens collected through sentinel surveillance. Using a Cox proportional hazards model with mixed effects, we estimated hazard ratios (HR) for hospitalization risk following infection with a variant, adjusting for age, sex, calendar week, and vaccination.
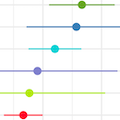
Findings: 58,848 cases were sequenced through sentinel surveillance, of which 1705 (2.9%) were hospitalized due to COVID–19. Higher hospitalization risk was found for infections with Gamma (HR 3.20, 95% CI 2.40–4.26), Beta (HR 2.85, 95% CI 1.56–5.23), Delta (HR 2.28 95% CI 1.56–3.34) or Alpha (HR 1.64, 95% CI 1.29–2.07) compared to infections with ancestral lineages; Omicron (HR 0.92, 95% CI 0.56-1.52) showed no significant difference in risk. Following Alpha, Gamma, or Delta infection, unvaccinated patients show higher hospitalization risk, while vaccinated patients show no significant difference in risk, both compared to unvaccinated, ancestral lineage cases. Hospitalization risk following Omicron infection is lower with vaccination.
Conclusion: Infection with Alpha, Gamma, or Delta results in a higher hospitalization risk, with vaccination attenuating that risk. Our findings support hospital preparedness, vaccination, and genomic surveillance.